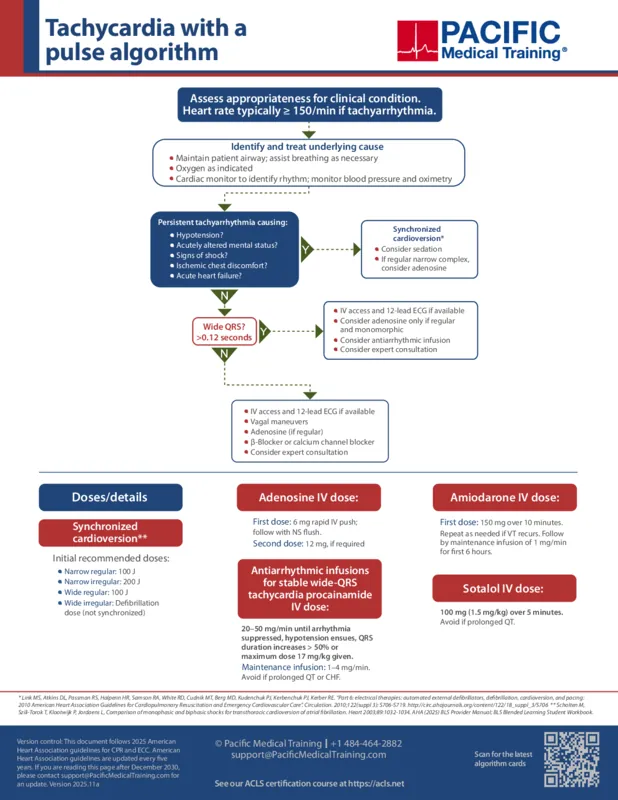
ACLS tachycardia algorithm: Managing stable tachycardia
 Written by Judy Haluka
Written by Judy Haluka
Changes: Updated tachycardia algorithm text per reviewer edits
For tachycardia, assess appropriateness for clinical consideration and treat the underlying cause. Tachycardia is a heart rate over 150 beats per minute. Maintain an open airway and assist ventilation as necessary. Administer oxygen if hypoxic. Place the patient on a cardiac monitor to identify the rhythm and to monitor blood pressure and oxygen saturation (SpO2).
Get ACLS certified
Our online course covers this algorithm and more. Earn up to 8 CME/CE credits.
Start ACLS course — $175Printed crash cart cards

Order the full set of printed crash cart cards.
Persistent tachycardia can cause hypotension, acutely altered mental status, signs of shock, ischemic chest discomfort, and acute heart failure. If the patient is having any of these signs, consider emergent synchronized cardioversion, follow your manufacturer's guidelines. Consider sedation prior to cardioversion, but do not delay treatment. If the rhythm is regular with narrow complexes, consider adenosine 6 mg IV rapid push.
If the patient is stable, measure the QRS. If QRS is wider than 0.12 seconds, establish IV access and obtain a 12-lead ECG. Consider adenosine only if the rhythm is regular and monomorphic. Consider IV antiarrhythmic infusions such as procainamide, amiodarone, or sotalol. Consider an expert consultation.
If QRS is less than 0.12 seconds, establish IV access and obtain a 12-lead ECG. If the rhythm is regular, encourage the patient to try a vagal maneuver. Administer adenosine 6 mg IV as a rapid push if the rhythm is regular. Consider a beta-blocker or a calcium channel blocker, and seek expert consultation.
For synchronized cardioversion, follow your manufacturer's guidelines. Initial recommended doses for a narrow regular rhythm (SVT) are 100 Joules. For narrow irregular rhythm (atrial fibrillation or atrial flutter) use 200 Joules. For a wide and regular rhythm, use 100 Joules. For a wide irregular rhythm, treat as ventricular fibrillation with immediate unsynchronized defibrillation at 200 Joules biphasic or 360 J monophasic.
Adenosine is given as a rapid IV push. First dose is 6 mg followed by a normal saline flush. If a second dose is required, give 12 mg IV rapid push.
Antiarrhythmic infusions for a stable wide-QRS include Procainamide, Amiodarone, or Sotalol IV. Procainamide dose is 20–50 mg/min until the arrhythmia is suppressed, the patient becomes hypotensive, the QRS duration increases more than 50%, or the maximum dose of 17 mg/kg is reached. Followed by a maintenance infusion of 1–4 mg/min. Avoid Procainamide if QT is prolonged or the patient has signs of heart failure. Amiodarone is given as a first dose of 150 mg over 10 minutes. Repeat as needed if VT recurs. Followed by a maintenance infusion of 1 mg/min for the first 6 hours. Sotalol is given 100 mg (1.5 mg/kg) over 5 minutes. Avoid if the patient has a prolonged QT.

Planning to certify/recertify ACLS?
Get a reminder when you need to take the exam
Please verify or enter a different email address:
How we reviewed this article
Our experts continually monitor the medical science space, and we update our articles when new information becomes available.
- Current versionMail the author of this pageEmail
- Feb 19, 2026
Reviewed by:
Changes: Updated tachycardia algorithm text per reviewer edits- Jul 1, 2021
Written by: